Leg Length Discrepancy And Shoe Lifts

Leg length inequality goes typically undiscovered on a daily basis, yet this problem is easily fixed, and can reduce many incidents of lower back pain.
Therapy for leg length inequality typically involves Shoe Lifts. They are low-priced, generally being below twenty dollars, in comparison to a custom orthotic of $200 plus. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Chronic back pain is easily the most prevalent condition affecting people today. Around 80 million men and women are affected by back pain at some stage in their life. It is a problem that costs employers millions annually on account of time lost and production. Innovative and more effective treatment solutions are always sought after in the hope of lowering economic influence this issue causes.

Men and women from all corners of the world suffer from foot ache as a result of leg length discrepancy. In a lot of these situations Shoe Lifts can be of very useful. The lifts are capable of eliminating any pain in the feet. Shoe Lifts are recommended by numerous certified orthopaedic doctors.
To be able to support the human body in a well balanced manner, your feet have a critical task to play. Inspite of that, it is sometimes the most neglected region of the human body. Some people have flat-feet which means there may be unequal force placed on the feet. This will cause other body parts like knees, ankles and backs to be impacted too. Shoe Lifts ensure that suitable posture and balance are restored.
Chiropodists Prefer Shoe Lifts For Leg Length Imbalances

Leg length inequality goes typically undiscovered on a daily basis, yet this problem is simply solved, and can eradicate numerous incidents of low back pain.
Treatment for leg length inequality typically consists of Shoe Lifts. Most are cost-effective, in most cases being less than twenty dollars, in comparison to a custom orthotic of $200 or higher. Differences over a quarter inch can take their toll on the spine and should probably be compensated for with a heel lift. In some cases, the shortage can be so extreme that it requires a full lift to both the heel and sole of the shoe.
Lumbar pain is the most common health problem impacting men and women today. Over 80 million men and women are affected by back pain at some point in their life. It is a problem that costs companies millions of dollars each year because of time lost and output. Fresh and more effective treatment methods are constantly sought after in the hope of reducing the economical impact this issue causes.

Men and women from all corners of the earth suffer from foot ache as a result of leg length discrepancy. In most of these situations Shoe Lifts can be of immense help. The lifts are capable of relieving any pain and discomfort in the feet. Shoe Lifts are recommended by many qualified orthopaedic doctors.
So as to support the body in a nicely balanced fashion, the feet have a very important part to play. Inspite of that, it can be the most overlooked zone in the human body. Some people have flat-feet meaning there may be unequal force placed on the feet. This causes other areas of the body such as knees, ankles and backs to be impacted too. Shoe Lifts ensure that the right posture and balance are restored.
Do Hammer Toe Splints Work
 Overview
Overview
There are two types of Hammer toes, Flexible hammertoes. If the toe still can be moved at the joint, it's a flexible hammertoe. That's good, because this is an earlier, milder form of the problem. There may be several treatment options. Rigid hammertoes. If the tendons in the toe become rigid, they press the joint out of alignment. At this stage, the toe can't be moved. It usually means that surgery is needed.
Causes
Flat feet can result in hammertoes, this is due to poor mechanics off the foot. High arched feet can also result in buckling toes. A major cause is in hereditary, all the toe conditions mentioned could be acquired due in hereditary factors. Bunions are a major cause of hammertoes. Claw toes are usually the result of a shoe that is too short. For many people, the second toe is actually longer than the great toe, and if shoes are sized to fit the great toe, the second (and maybe even the third toe) will have to bend to fit into the shoe. Shoes that are pointed make matters even worse. Combine pointed shoes with high heels, the foot is under similar pressure as if it was constantly being pushed downhill into a wall. Rheumatoid arthritis can also lead to bunions, which in turn can lead to hammer toes.
A hammertoe causes you discomfort when you walk. It can also cause you pain when trying to stretch or move the affected toe or those around it. Hammertoe symptoms may be mild or severe. Mild Symptoms, a toe that is bent downward, corns or calluses. Severe Symptoms, difficulty walking, the inability to flex your foot or wiggle your toes, claw-like toes. See your doctor or podiatrist right away if you develop any of these symptoms.
Diagnosis
Most health care professionals can diagnose hammertoe simply by examining your toes and feet. X-rays of the feet are not needed to diagnose hammertoe, but they may be useful to look for signs of some types of arthritis (such as rheumatoid arthritis) or other disorders that can cause hammertoe. If the deformed toe is very painful, your doctor may recommend that you have a fluid sample withdrawn from the joint with a needle so the fluid can be checked for signs of infection or gout (arthritis from crystal deposits).
Non Surgical Treatment
Your podiatrist may recommend conservative treatment techniques for your hammertoes based on your foot structure, which will likely involve removing hammertoe any thick, painful skin, padding your painful area, and recommending for you shoes that give your curled toes adequate room. Conservative care strategies for this health purpose may also involve the use of Correct Toes, our toe straightening and toe spacing device.
Surgical Treatment
Several surgical procedures are available to the podiatric physician. For less severe deformities, the surgery will remove the bony prominence and restore normal alignment of the toe joint, thus relieving pain. Severe hammertoes, which are not fully reducible, may require more complex surgical procedures. Recuperation takes time, and some swelling and discomfort are common for several weeks following surgery. Any pain, however, is easily managed with medications prescribed by your podiatric physician.
Causes Of Bunions
Overview
 A bunion (hallux valgus) is a deformity of the base joint of the big toe. The cause is not clear in many cases. The deformity may cause the foot to rub on shoes, which may cause inflammation and pain. Good footwear is often all that is needed to ease symptoms. An operation to correct the deformity is an option if good footwear does not ease symptoms.
A bunion (hallux valgus) is a deformity of the base joint of the big toe. The cause is not clear in many cases. The deformity may cause the foot to rub on shoes, which may cause inflammation and pain. Good footwear is often all that is needed to ease symptoms. An operation to correct the deformity is an option if good footwear does not ease symptoms.
Causes
Although they may develop on the fifth (little) toe, bunions usually occur at the base of the big toe. Bunions are often caused by incorrect foot mechanics. The foot may flatten too much, forcing the toe joint to move beyond normal range. In some cases, joint damage caused by arhritis or an injury produces a bunion. And some people are simply born ith extra bone near a toe joint. If you're at risk for developing a bunion, wearing high-heeled or poorly fitting shoes make the problem worse. As new bone grows, the joint enlarges. This stretches the joint's outer covering. Force created by the stretching pushes the big toe toward the smaller ones. Eventually, the inside tendons tighten, pulling the big toe farther out of alignment.
Symptoms
Corns and calluses may occur on the soles of the feet, in between toes and on the bunion joint. Stiffness can occur at the big toe due to secondary arthritis, this is known as Hallux Rigidus. Other foot conditions can occur such as in growing toenails and in severe cases the bunion joint may have a fluid filled sack called a bursitis. This can be very painful and can become infected.
Diagnosis
Although bunions are usually obvious from the pain and unusual shape of the toe, further investigation is often advisable. Your doctor will usually send you for X-rays to determine the extent of the deformity. Blood tests may be advised to see if some type of arthritis could be causing the pain. Based on this evaluation, your doctor can determine whether you need orthopaedic shoes, medication, surgery or other treatment.
Non Surgical Treatment
There are many treatment options for bunions and they will vary with the type and severity of each bunion and will also depend on what is causing the symptoms. Bunions are almost always progressive and tend to get larger and more painful with time, how fast this happens may be a function of the fit of the footwear. The initial goal of treatment options is to relieve pressure on the bunion and any symptoms that may be present and to halt or slow the progression of the joint deformity. There is no effective may be "get rid off" a bunion without surgery. There are a number of things that individuals and Podiatrists can do to help the symptoms and slow (if not halt) progression. 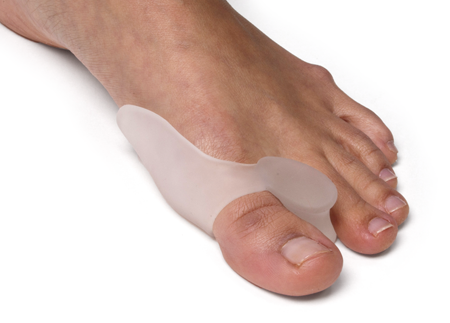
Surgical Treatment
If your bunion is symptomatic and causing you persisting and troublesome symptoms then surgery should be considered. There is no correct amount of pain or inconvenience which a bunion may cause which warrants surgery. Symptoms which a bunion causes are generally subjective, and what is a problem in one person?s view will not be a problem in another's. For bunion surgery to be successful (correcting the deformity and losing the symptoms) the mechanical factors driving the deformity should be overcome. Bunion surgery should replace the 1st metatarsal closer to the 2nd thus reducing the width of the foot, and also realigning the tendons and reducing their deforming forces. These principals of bunion surgery are well demonstrated by the following x-rays which shows how a Scarf osteotomy has achieved this aim.
Prevention
If the diagnosis is made early on, such as in preadolescence, bunion development can be slowed and in some cases arrested with the proper supportive shoe gear and custom functional shoe inserts (orthotics). Avoidance of certain athletic activities with improper shoe fit and toe pressure can prevent the symptoms that occur with bunions.
What Will Be The Indications Of An Achilles Tendon Rupture
Overview
 The Achilles tendon is situated above the heel and forms the lower part of the calf muscles. It is a continuation of the two calf muscles, the gastrocnemius and soleus muscles, and it attaches to the heel bone. It is the strongest tendon in the human body and must withstand great forces. Its function is to transmit the force produced by the calf muscles to lift the heel and produce the push off during walking, running and jumping. The Achilles can produce force of up to seven times body weight. This shows just how much force it has to withstand during sporting activities, such as sprinting, jumping and turning.
The Achilles tendon is situated above the heel and forms the lower part of the calf muscles. It is a continuation of the two calf muscles, the gastrocnemius and soleus muscles, and it attaches to the heel bone. It is the strongest tendon in the human body and must withstand great forces. Its function is to transmit the force produced by the calf muscles to lift the heel and produce the push off during walking, running and jumping. The Achilles can produce force of up to seven times body weight. This shows just how much force it has to withstand during sporting activities, such as sprinting, jumping and turning.
Causes
Ruptured Achilles tendons may result from falling from a height or down a hole. Increasing training intensity abruptly, boosting distance, frequency or duration by more than 10% a week. Failing to stretch before and after exercise. Repetitive training, especially uphill running. Deyhydration, which causes cramping and tightness in the calves. Taking antibiotics. Improper footwear. Explosive movements in competitive sports like basketball, soccer or track & field.
Symptoms
A person with a ruptured Achilles tendon may experience one or more of the following. Sudden pain (which feels like a kick or a stab) in the back of the ankle or calf, often subsiding into a dull ache. A popping or snapping sensation. Swelling on the back of the leg between the heel and the calf. Difficulty walking (especially upstairs or uphill) and difficulty rising up on the toes. These symptoms require prompt medical attention to prevent further damage. Until the patient is able to see a doctor, the "R.I.C.E." method should be used. This involves, rest. Stay off the injured foot and ankle, since walking can cause pain or further damage. Ice. Apply a bag of ice covered with a thin towel to reduce swelling and pain. Do not put ice directly against the skin. Compression. Wrap the foot and ankle in an elastic bandage to prevent further swelling. Elevation. Keep the leg elevated to reduce the swelling. It should be even with or slightly above heart level.
Diagnosis
Your caregiver will ask what you were doing at the time of your injury. You may need any of the following. A calf-squeeze test is used to check for movement. You will lie on your stomach on a table or bed with your feet hanging over the edge. Your caregiver will squeeze the lower part of each calf. If your foot or ankle do not move, the tendon is torn. An x-ray will show swelling or any broken bones. An ultrasound uses sound waves to show pictures of your tendon on a monitor. An ultrasound may show a tear in the tendon. An MRI takes pictures of your tendon to show damage. You may be given dye to help the tendon show up better. Tell the caregiver if you have ever had an allergic reaction to contrast dye. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the caregiver if you have any metal in or on your body.
Non Surgical Treatment
Treatment for a ruptured Achilles tendon often depends on your age, activity level and the severity of your injury. In general, younger and more active people often choose surgery to repair a completely ruptured Achilles tendon, while older people are more likely to opt for nonsurgical treatment. Recent studies, however, have shown fairly equal effectiveness of both operative and nonoperative management. Nonsurgical treatment. This approach typically involves wearing a cast or walking boot with wedges to elevate your heel, which allows your torn tendon to heal. This method avoids the risks associated with surgery, such as infection. However, the likelihood of re-rupture may be higher with a nonsurgical approach, and recovery can take longer. If re-rupture occurs, surgical repair may be more difficult. 
Surgical Treatment
Thanks to a new surgical technique, operative procedures are often more beneficial.The operative treatment of Achilles tendon ruptures has significantly changed in recent years. The objective today is to connect the torn tendons using modern suture and possibly adhesive materials. Through small surgical incisions the ends of the torn tendon are surgically exposed, and sutures are used to tie the ends permanently together. Thus, the operated repaired tendon is again resilient within a reasonable time. The cast treatment and walking on crutches required in the past, is with this procedure usually not necessary. Instead, functional treatment following the surgery involves wearing a special boot, meaning that the patient can put weight onto the operated leg again within a few days after surgery. Physical therapy training will start immediately following the operation. The philosophy behind such an early functional treatment is that tissue adequately adapts to stress and thus accelerates the healing process. For the patient, the modern surgical treatment of an Achilles tendon rupture has the distinct advantage that no prolonged hospital stay is necessary. Hospital stay usually lasts only a few days. Using crutches, patients can return to work soon after the surgery.